
With Stroke, Think FAST
May is National Stroke Month.
The purpose is to increase awareness of what you can do to reduce your risk of a stroke and what you should do if you suspect someone is having a stroke.

May is National Stroke Month.
The purpose is to increase awareness of what you can do to reduce your risk of a stroke and what you should do if you suspect someone is having a stroke.
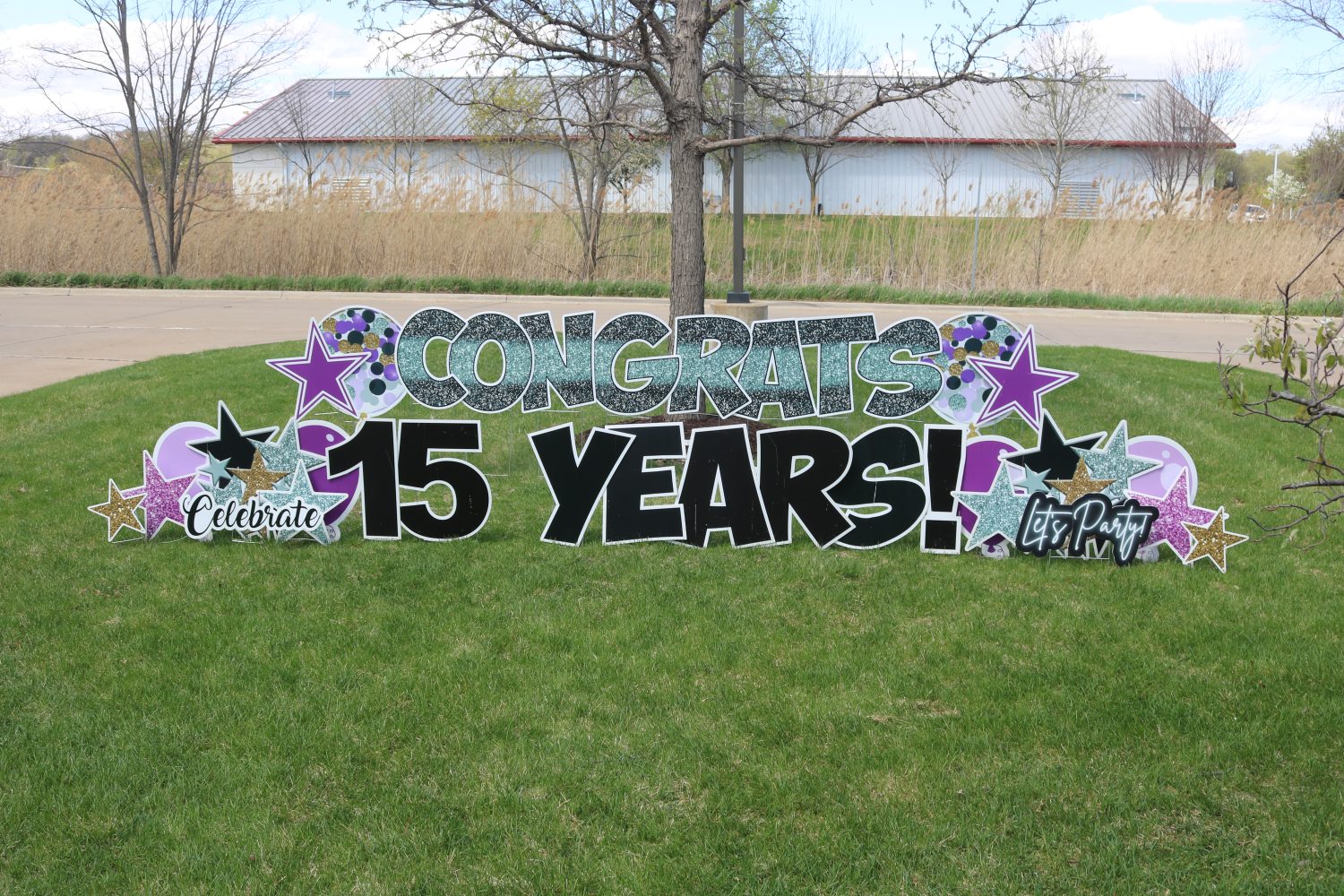
Heritage Woods of Moline celebrated their 15 year anniversary this past Friday. Over the past 15 years, Heritage Woods of Moline has had the opportunity to serve more than 750 residents.
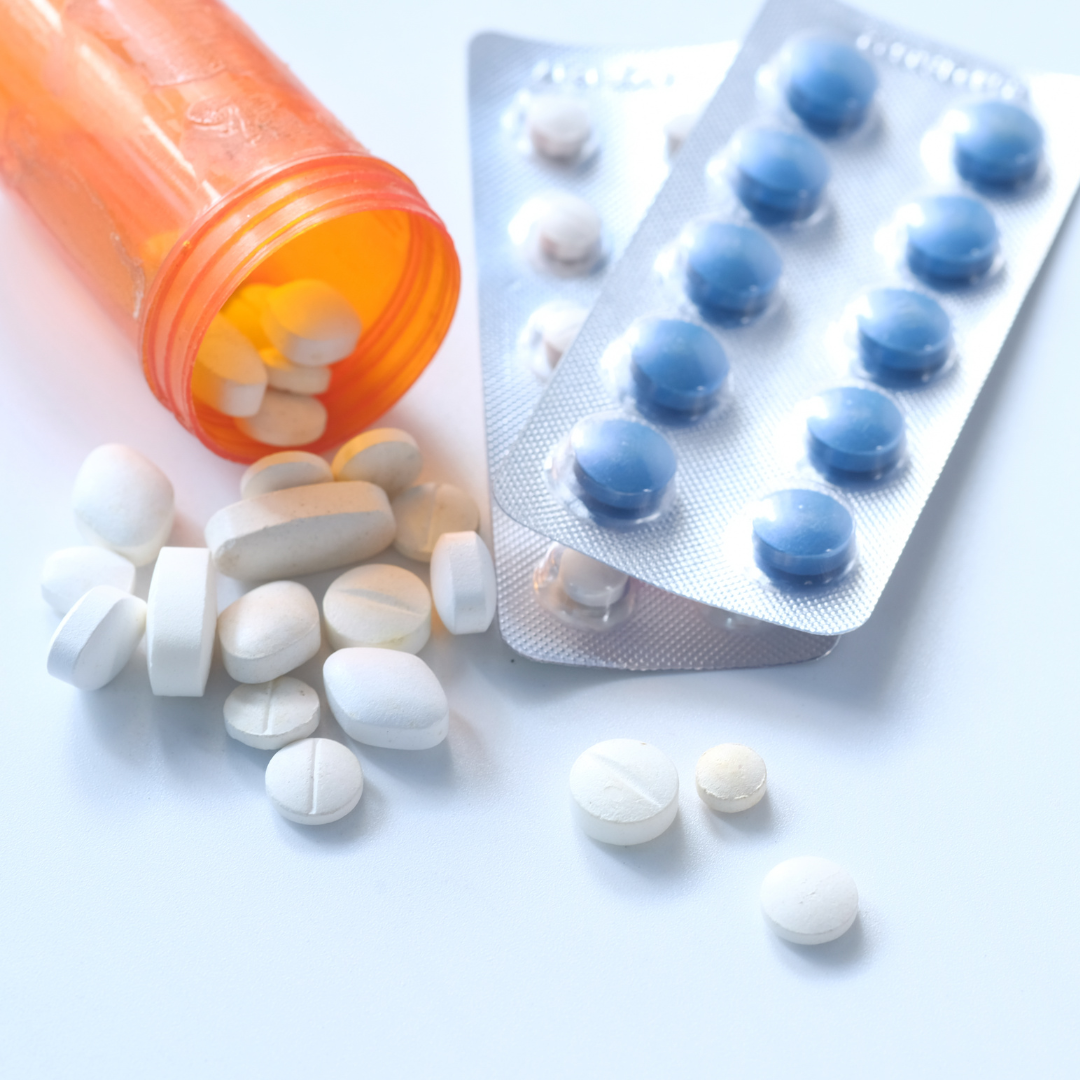
On Saturday, April 22, you have a chance to safely and anonymously dispose of any expired, unneeded or unwanted medications that you have.
It is a National Prescription Drug Take-Back Day sponsored by the U.S. Department of Drug Enforcement (DEA).
Twice each year, the DEA in partnership with local law enforcement hosts a National Prescription Drug Take-Back Day.

James had been looking for a place to live for a very long time, but could not find housing that

In 1987, President Ronald Reagan signed a proclamation designating March as National Disability Awareness Month. The proclamation created a special opportunity to raise awareness about the support needed by persons with disabilities as well as their right to enjoy life and to feel productive and secure.
In her book “Breaking the Age Code,” author Becca Levy, Ph.D., highlights through data and stories the reasons why we need to combat ageism and details strategies that all of us can use to bolster positive beliefs about aging.

Each year in January, we celebrate National Thank You Month. It is a time to show gratitude, express appreciation, and thank others for the little and the big things they have done to make life better.

Evergreen Village of Bloomington and Heritage Woods of Flora were honored as Gardant’s 2022 Communities of the Year!

The period of time from Thanksgiving to New Year’s Day can be hectic. On top of everything else you have to do, there is the decorating, shopping, cooking, gift wrapping, get-togethers with family and friends, and holiday parties. At the same time, the holiday season can be the perfect time of year to consider assisted living.

November is National Gratitude Month. It is a time to reflect on what we are grateful for; a time to celebrate and give thanks for our many blessings. Throughout the month, we are posting Blogs that feature the thoughts on gratitude from residents and staff of the senior living, assisted living, supportive living, and memory care communities Gardant operates. Click to read Chapter 8!

November is National Gratitude Month. It is a time to reflect on what we are grateful for; a time to celebrate and give thanks for our many blessings.Throughout the month, we are posting Blogs that feature the thoughts on gratitude from residents of the senior living, assisted living, supportive living, and memory care communities Gardant operates. Click to read Chapter 7!

November is National Gratitude Month. It is a time to reflect on what we are grateful for; a time to celebrate and give thanks for our many blessings.Throughout the month, we are posting Blogs that feature the thoughts on gratitude from residents of the senior living, assisted living, supportive living, and memory care communities Gardant operates. Click to read chapter 6!
4882 North Convent Street
Bourbonnais, Illinois 60914
877.882.1495
info@gardant.com
"*" indicates required fields
Gardant Management Solutions has 20+ years of industry-acclaimed operational history in developing, managing and consulting for senior living, assisted living and memory care communities.